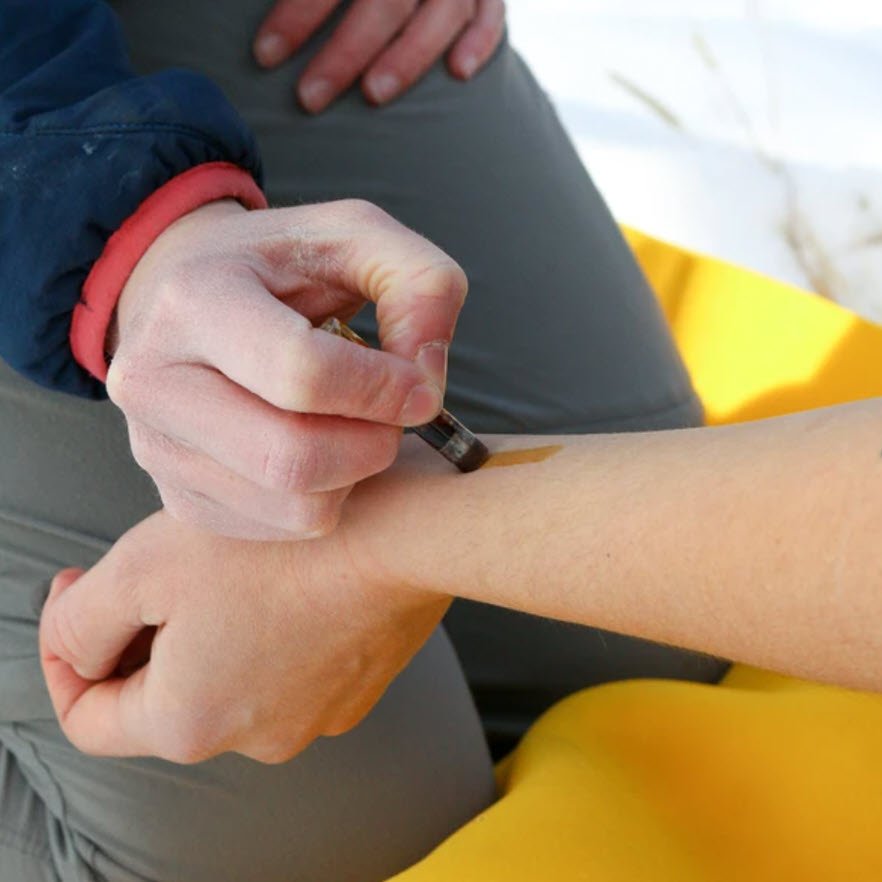
Is it possible to toughen your feet as a way of preventing foot blisters? If so, how do you do it? Do black tea soaks really work? I'm happy to report that yes, you can toughen your skin. But it might be a little different than you think. Get ready for a discussion about the adaptive changes that occur within your skin, callouses, pre-conditioning your feet and how long it takes, and finally, commonly-used "skin toughening" products.
Skin Toughening Occurs By Adaption On A Cellular Level
Skin adapts to the forces placed upon it. Early research by MacKenzie in 1974 found that when the skin is subjected to repeated low level frictional forces, the following changes occur:
- Epidermal cell turnover is faster
- Cells are more resistant to frictional forces
- And the epidermis becomes thicker
What's more, these skin toughening adaptive changes in the epidermis take place sooner than you might think. MacKenzie (1974) examined changes to the skin of mouse ears that were rubbed every day 10 times with a moderate force (so as not to cause skin damage). Skin characteristics were observed at day 1, 7, 14, 28 and 35. What MacKenzie found, in fact, was there were more cells in the epidermis. And they were larger and more resistant to mechanical damage, compared to ears that received no rubbing. The interesting thing to note was, the changes at 7 days were identical to those at 14, 28 and 35 days. And this was with just 10 rubs of moderate force per day!
Sanders et al (1995) reviewed the literature on the skin's response to shear and friction. This included studies conducted on the skin of the palms (Bennett et al, 1979), thigh (Rubin, 1949), anterior tibial surface (Naylor, 1955 ), back, buttocks, shins, forearms upper arms, thighs, palms and soles (Sulzberger et al, 1966), the palms and soles of monkeys (Cortese et al, 1969), mouse ears (MacKenzie, 1974 ) and rat gums (Carter, 1956). They summarise the adaptive changes leading to increased resistance to epidermal fatigue:
The results suggest mechanisms and processes for adaptation to frictional stress. The cells at the basement membrane increase in size, density, and speed of transport across the epidermis, increasing thickness of the stratum corneum layer. The thickened stratum corneum means that there is a greater volume through which to distribute the shear load between the skin surface and immediately above the basement membrane. With a greater volume of stratum corneum, shear stress gradients are lower; thus, the skin is at lower risk of failure.
Wang and Sanders (2003) reviewed the literature on this topic to form an understanding the adaption process on a molecular level. Specifically, the 2003 paper had a focus of developing biomolecule delivery strategies to prevent another skin shear injury occurring commonly in lower-limb amputees wearing prosthetic limbs. They concluded that adaption of the skin to mechanical stresses (ie: shear distortions) occurs by forming new collagen fibrils with larger diameters, as opposed to increasing diameters of existing fibrils. At the same time, there is breakdown of existing small diameter fibrils.
Their review suggested that within 4 days of mechanical stress application (ie: shear stress), the adaption process starts with synthesis and activation of metalloproteinases and the breakdown of some existing collagen fibrils. Then at least 7 days after the first application of stress, the new proteoglycan environment would induce the formation of collagen fibrils with larger diameters.
Callouses
We know that both blisters and callouses are caused by repetitive shear distortions. A callous is the adaptive manifestation of chronic shear stress that remains below the threshold for mechanical fatigue. If above that threshold, the intraepidermal tear precipitating blister formation will be the result.
Taking into account the words of Sanders et al in their 1995 paper, increased stratum corneum thickness (ie: callous) distributes shear stress over a larger area thereby reducing shear stress gradients and affecting some level of blister prevention. So callous is an advantage.
However, there are degrees of callous. As tempting as it might sound, the building of thick chunky callouses over blister prone areas is ill-advised. Excessively thick callouses are not entirely protective of blister formation. What's more, they can make blisters very difficult to deal with. Read this article for more about callouses and blisters.
Certainly, if blisters were a superfical-to-deep wear injury, a very thick corneum would be beneficial. Because it would take longer to wear through all that extra skin. But remember, blisters are not a superfical-to-deep wear injury. They are a shear stress injury - a mechanical fatigue underneath the skin surface caused by excessive repetitive shear.
Pre-Conditioning and Breaking In Shoes
The adaptive changes that occur to your skin require that you subject your feet to very forces that threaten to damage it. For blisters, that is shear distortions. It can be a fine line. Here's what the research shows about time spent in your shoes, training and blister incidence:
- Van Tiggelen et al (2009) found previous hiking or military experience offered some protection to blister formation in 189 recruits going through basic military training.
- Thompson et al (1993) studied blister incidence in 357 male Marine recruits undergoing basic training over 12 weeks. They concluded that blisters were most noticeable early on in recruit training, when “recruits are adapting to the rigours of physical training and acquiring their military skills.”
- Brennan et al (2012) reports that during a 12 month deployment in Iraq, troops who did not “break in” their boots were more likely to suffer with blisters.
- Patterson et al (1994) studied foot blister risk factors in military cadets who underwent an abrupt increase in walking, running and general physical activity during 6 weeks of summer Army Reserve Officer Training Corps training. Those that wore their boots less than 20 hours per week in the 2 weeks leading up to training were more likely to get foot blisters.
- Gardner and Hill (2002) found hikers who had not preconditioned their footwear were more likely to get blisters (32% versus 25%).
- Jagoda et al (1981) looked at a group of 221 male lieutenants taking part in their first training hike and found the likelihood of blister formation depended on the running habits of the individual. Incidence of blisters was highest in the early rather than later stages of training, suggesting adaptive changes took time to occur. In addition, incidence of blisters was highest in the early stages of training, indicating that adaptive changes took time to occur.
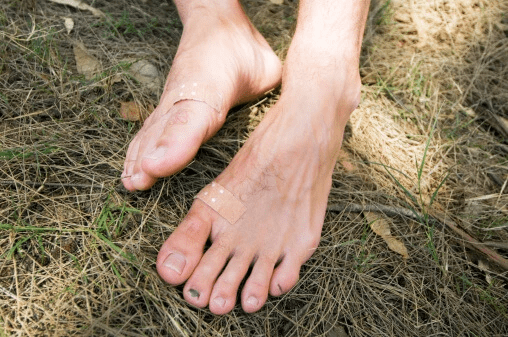
How Long Does It Take For The Skin To Toughen?
- The Thompson et al (1993) study mentioned in the above paragraph found highest blister incidence in weeks 1-3 compared to weeks 4-6, weeks 7-9 and weeks 10-12. This suggests the skin adapts to the shear loads of this activity somewhere within the first 3 weeks.
- The Patterson et al (1994) study mentioned above found 95% of all blister cases occurred in the first 3 weeks of the 6-week training, with 86% occurring in the first 2 weeks (Week 1 = 34.6%; Week 2 = 51.2%; Week 3 = 9.3%). This suggests adaption occurs somewhere within the first 2-3 weeks.
- Choi et al (2013) also found the majority of blisters occurred on day 2 - see graph below. A group of 142 Korean college student volunteers undertook a 21 day, 580km road march. Just over 95.1% of students developed their first foot blister in the first 5 days. This suggests that in this population, the skin adapts to this activity within 5 days.
- Reynolds et al (1999) looked at injury rates of 218 light infantry soldiers over a 5-day 161km cross-country march. They determined the majority of blisters occurred on day 2 (from 32km to 65km) and no blisters occurred on days 4 or 5 (from 97km to 161km) - see table below. This suggests the skin adapts to these shear loads after 2-4 days.
- Lipman et al (2014) and Lipman et al (2016) found blisters occurred by the end of day 2 in 89% and 80% respectively of 155-mile ultramarathons participants. This is suggests adaption to this type of activity occurs within the first 2 days.
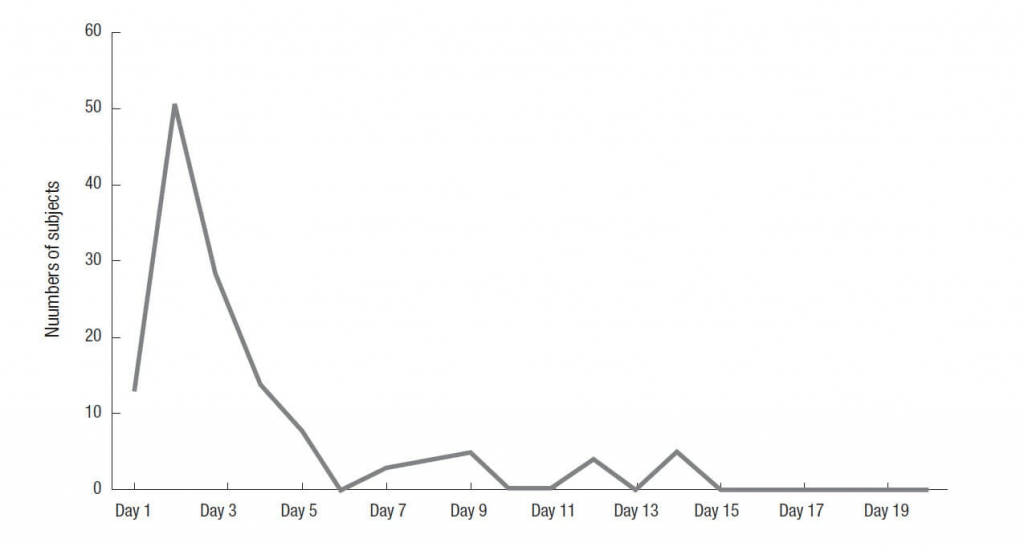 Ninety percent of blisters occurred within the first five days, with blister incidence highest on day two (Choi et al, 2013).
Ninety percent of blisters occurred within the first five days, with blister incidence highest on day two (Choi et al, 2013).
As a side-note, there were less than ideal aspects to the Korean 21-day hiking event. Shoes were provided to all participants and for some reason, cotton socks were worn in spite of an average humidity of 93%... what were they thinking?
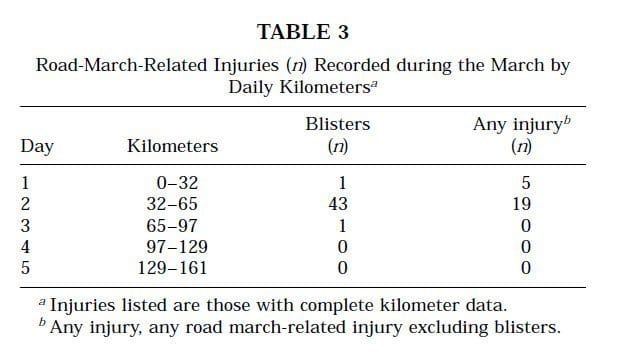
Reynolds et al (1999) Injuries and Risk Factors in a 100-Mile (161-km) Infantry Road March
Is It Skin Toughening Or Skin Drying?
Skin toughening is a phrase commonly used by runners and hikers to describe the effect of astringent preparations. For example, alcohol foot soaks, salt water or black tea foot baths, Friars Balsam, Akileine Tano and others (Read, 1990; Vonhof, 2012). However, an exact blister preventive "skin toughening" mechanism of action is not clear. In fact, it hasn't even attracted any expert commentary, that I can find. And there's no blister or skin friction research that has tested these astringent preparations (Knapik et al, 1995).
One thing I can tell you is these astringents do have a "skin drying" effect. Very dry skin, rather than moist skin, certainly means lower friction levels. And we know that means less blisters. But does it mean tough skin? Probably not. Not in an in-shoe environment where one is exercising. It won't take long for the skin to become something other than "very dry".
The Limitations of Adaption
Depending on your individual blister threshold, this protective mechanism of skin adaption may not provide full blister protection. The research results quoted earlier show a somewhat reduced blister incidence, but in many cases, not a zero blister incidence.
Conclusion
Whether it's new shoes, different activities, longer distances or more challenging terrains - they all exert new shear loads to the skin. Getting your skin used to these new stresses by making incremental changes can help protect your skin and make it more able to resist blister formation ... to a point. Maximise it, but realise you may need to implement other preventive strategies on top of the adaptive process.
References
- Van Tiggelen D, Wickes S, Coorevits P, Dumalin M and Witvrouw E. 2009. Sock systems to prevent foot blisters and the impact on overuse injuries of the knee joint. Military Medicine. 174 (2): 183-9.
- Brennan FH, Jackson CR, Olsen C and Wilson C. 2012. Blisters on the battlefield: the prevalence of and factors associated with foot friction blisters during operation Iraqi freedom. Military Medicine. 177 (2): 157-162.
- Patterson HS, Woolley TW and Ledner WM. 1994. Foot blister risk factors in an ROTC summer camp population. Military Medicine. 159(2): 130-5.
- Thompson KJ, Hamlet MP, Jones BH and Knapik JJ. 1993. Impact of sock systems on frequency and severity blister injury in a marine recruit population. US Army Research Institute of Environmental Medicine. Technical Report No. 6(93): 1-44.
- Gardner TB and Hill DR. 2002. Illness and injury among long-distance hikers on the long trail, Vermont. Wilderness and Environmental Medicine. 13: 131-134.
- Mackenzie IC. 1974(A). The effects of frictional stimulation on mouse ear epidermis I. Cell proliferation. The Journal of Investigative Dermatology. Vol 63 No 2: 80-85.
- Mackenzie IC. 1974(B). The effects of frictional stimulation on mouse ear epidermis II. Histological appearance and cell counts. The Journal of Investigative Dermatology. Vol 63 No2: 194-198.
- Jagoda A, Madden H and Hinson CA. 1981. Friction blister prevention study in a population of marines. Military Medicine. 146(1): 42-44
- Sanders JE, Goldstein BS and Leotta DF. 1995. Skin response to mechanical stress: adaptation rather than breakdown – a review of the literature. Journal of Rehabilitation Research and Development. Vol 32 No 3 (October): 214-226.
- Knapik JJ, Hamlet MP, Thompson KJ and Jones BH. 1996(A). Influence of boot-sock systems on frequency and severity of foot blisters. Military Medicine. 161(10): 594-598.
- Knapik JJ, Harman E and Reynolds K. 1996(B). Load carriage using packs: a review of physiological, biomechanical and medical aspects. Applied Ergonomics. Vol 27 No 3: 207-216
- Wang Y & Sanders J. 2003. How does skin adapt to repetitive mechanical stress to become load tolerant? Medical Hypotheses. 61 (1), 29-35.
- Choi S-C, Min Y-G, Lee I-S, Youn G-H, Kang B-R, Jung Y-S, Cho J-P and Kim G-W. 2013. Injuries associated with the 580km university student grand voluntary road march: focus on foot injuries. Rehabilitation and Sports Medicine. Journal of Korean Medical Science. 28: 1814-1821.
- Reynolds KL, White JS, Knapik JJ, Witt CE and Amoroso PJ. 1999. Injuries and risk factors in a 100 mile (161 km) infantry road march. Preventative Medicine. 28: 167-173.
- Read PJ. 1990. An Introduction to Therapeutics for Chiropodists. Exeter, A Wheaton & Co Ltd.
- Vonhof J. 2012. Fixing your feet – Injury prevention and treatment for athletes (5th edition). Birmingham, Wilderness Press.
- Knapik JJ, Reynolds K, Duplantis KL and Jones BH. 1995. Friction blisters – pathophysiology, prevention and treatment. Sports Medicine. Vol. 20(3): 136-147.
- Lipman, G. S., Sharp, L. J., Christensen, M., Phillips, C., DiTullio, A., Dalton, A., Ng, P., Shangkuan, J., Shea, K., & Krabak, B. J. (2016). Paper Tape Prevents Foot Blisters: A Randomized Prevention Trial Assessing Paper Tape in Endurance Distances II (Pre-TAPED II). Clinical journal of sport medicine : official journal of the Canadian Academy of Sport Medicine, 26(5), 362–368.
- Lipman, G. S., Ellis, M. A., Lewis, E. J., Waite, B. L., Lissoway, J., Chan, G. K., & Krabak, B. J. (2014). A prospective randomized blister prevention trial assessing paper tape in endurance distances (Pre-TAPED). Wilderness & environmental medicine, 25(4), 457–461.