Updated 2023: Most of us understand that foot blisters result from some combination of heat, moisture, and friction. While all three factors are relevant, this generalisation grossly over-simplifies the actual process. In fact, the perception one is left with is an inaccurate one. It should come as no surprise then that without an adequate understanding of what causes blisters on feet, obstacles to effective management are almost inevitable.
The old “what causes foot blisters” understanding
- Yes your foot gets hot in your shoe – that’s unavoidable.
- Yes, this makes your foot sweat – that’s unavoidable too.
- And yes, that moisture increases friction levels – that’s also unavoidable.
Try keeping your feet cool and dry in your shoes when you’re exercising even on a cool day – it’s impossible! But that doesn’t mean you have to get blisters – even if it’s really hot and humid, even if you’re on your feet all day, even if you’re really sweaty.
This article highlights the holes in the old heat-moisture-friction blister paradigm and offers a new paradigm for what causes blisters. One that is accurate, easy for the lay population to understand, repeatable and points us towards the array of opportunities for effective management practices.
Heat, moisture and friction
Heat is relevant to blister formation. While friction blisters are not a thermal burn,1–9 we know it is easier to get blisters in hot conditions compared to cold,5,10 that there is an increase in skin temperature preceding blister formation,8 and there is a prolonged increase in temperature after the blister forms.8 What’s more, higher temperatures cause more perspiration3 and unsurprisingly, faster walking speeds increase in-shoe temperatures11,12 and increased sweating.13 This perspiration that provides the ‘moist’ environment known to increase friction levels 2,14–16 and blister formation.3,17
The contradictory definitions of friction is responsible!
Friction is a fundamental factor to the cause of foot blisters, but is more counterintuitive than one might expect. Why? Because friction has two meanings. It means both rubbing, and the resistance to movement of one surface over another18 – two contradictory definitions.
In the case of foot blisters, it’s the first definition that the majority of us see in our mind’s eye when we think heat-moisture-friction. However, it’s the second definition of friction that we should be thinking of – the resistance to movement. The second definition means things rub less – there is more resistance to rubbing so it takes longer for movement to occur.
So, let’s examine both a low friction scenario and a high friction scenario and determine their relevance to the cause of foot blisters.
Low friction scenario:
Let’s take the greasy lubricant, Vaseline. It is often used on the feet to prevent blisters. Vaseline reduces the skin’s resistance to movement. It makes things more slippery. It reduces the coefficient of friction (COF). Vaseline reduces the friction level and allows things to slip/slide/rub/move across one another more easily. A low friction scenario is one where there is less resistance to movement so that things rub more. This is how lubricants (and other friction-reducing strategies) prevent blisters. Rubbing does not cause foot blisters. In fact, promoting rubbing by way of reduced friction levels is how you can prevent blisters.
High friction levels make things stick together for longer – an increased resistance to movement. For example, perspiration causes the skin to become clammy or tacky or sticky. It increases the COF. Sweaty feet increase friction levels and make it more difficult for things to slip or slide or rub or move across one another. If movement does happen, it happens much later. This is the increased friction levels that are unequivocally linked to the cause of blisters on feet.
But how, exactly?
Soft tissue shear distortions cause foot blisters via a mechanical fatigue
It has to do with soft tissue shear distortions (shear deformation). Higher friction levels make the skin, sock and shoe surfaces remain in stationary contact for longer, while the bones move back and forth within the foot as part of normal function. This results in larger shear distortions of all the soft tissues in between skin surface (not moving) and bone (moving). As the bones continue to move within the foot with each step, the skin does not immediately follow. And so the soft tissues in between undergo shear deformation. Picture the individual layers of skin and soft tissue gliding parallel over one another to allow for this skin-bone mismatch. The longer the skin remains stationary, the higher the shear distortion. These shear distortions, when repetitive, are known to cause blisters.1-4, 8,14,16,19–24
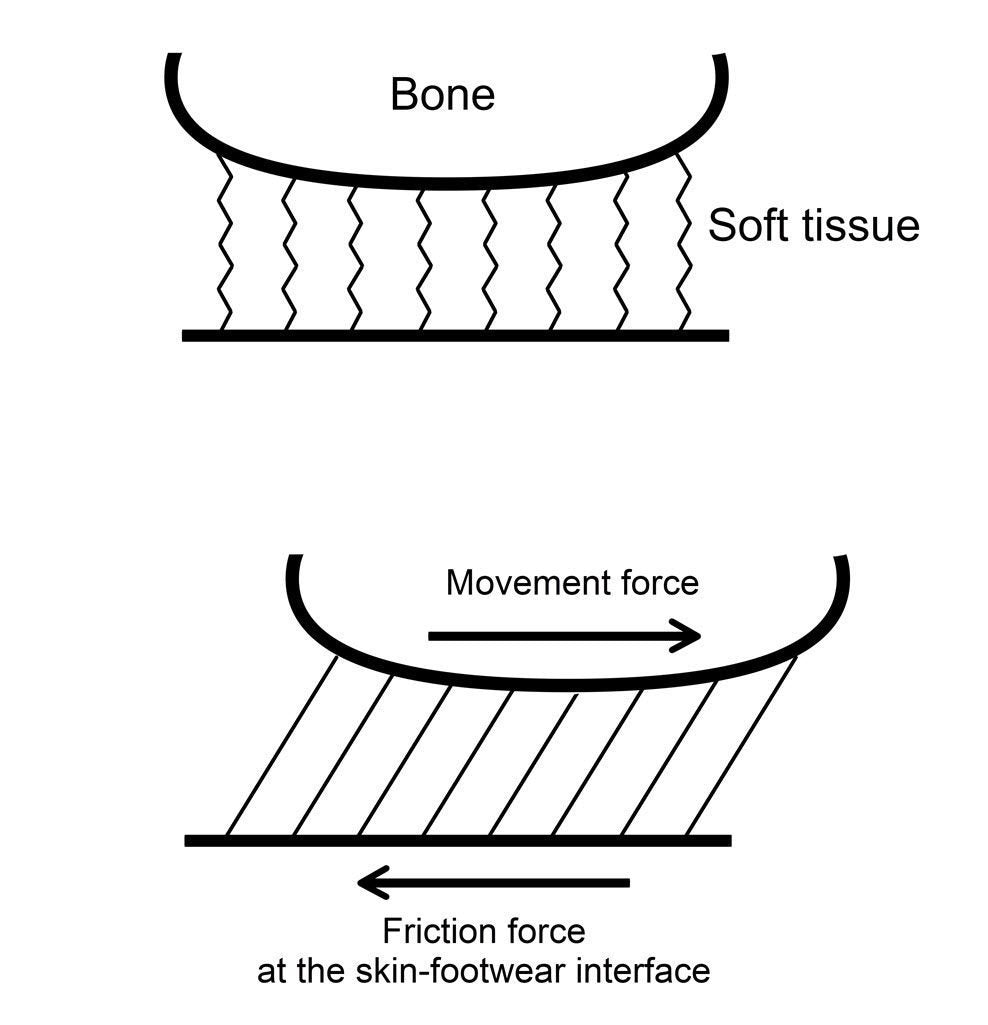
This is the crux of shear distortion
Doug Richie20 described it best when he mentioned the skin and bones moving out of sync with one another:
“These (shear) forces cause the skeletal segments of the foot to move out of synch with the overlying soft tissue and components of the shoe.”
Doug Richie, 2010
In my opinion, Richie’s is the best descriptive attempt to explain what shear distortions are – the skin and bones moving out of sync and everything in between undergoes shear distortion. You can see it happening in your mind’s eye. Now, ten years on, “skin and bone moving out of sync” now forms the basis of the new blister causation paradigm.
In addition, there needs to be a break in the habit of thinking blisters as a superficial-to-deep wear injury due to rubbing. Blisters start as a tear under the skin surface, within the epidermis at the level of the stratum spinosum.1–4,8,14,20,21,23,24 Comaish1 in particular investigated potential causes of this and determined the mechanism of injury as an “epidermal fatigue” due to repetitive shear forces. The tear is often referred to as a “cleft”. In the spirit of keeping things simple, I believe tear is better word as it’s in the common vernacular and widely understood.
The new “what causes foot blisters” paradigm
With the above in mind, a new paradigm has been proposed for foot blister causation by Rushton and Richie in 2023. As you can see, this is not new information; the existing body of research is unequivocal on what causes friction blisters on the feet. It’s simply an improvement on the current heat-moisture-friction paradigm by being:
- Accurate
- Brief and descriptive
- Easily understood by the lay population
- Less likely to be misinterpreted
The first sentence encapsulates cause and effect and can be used as the briefest answer to the question “what causes blisters”:
Blisters are a tear under the skin surface caused by the skin and bone moving out of sync.
The second and third sentences introduce and define shear distortion, the logical next point to make:
As the bones move within the foot with each step, the skin does not immediately follow, and so the soft tissues in between are made to stretch and distort. This is called shear distortion.
The fourth sentence describes the injury that is so familiar to us all:
If there is too much shear, a tear develops under the skin surface which later fills with fluid to become what we recognise as a blister.
A segue to how blister prevention works
The previous sentence begs the questions how much shear is too much. It provides a nice segue to a high-level overview of the opportunities for blister prevention if the conversation requires it.
The point at which the tear occurs under the skin surface is determined by, a) the number of shear distortions, b) the intrinsic resilience of the skin to shear distortion and, c) the magnitude of shear distortions.
To explain this last point a little further:
A more verbose explanation of “what causes foot blisters” might go something like this:
The foot doesn’t function like a block of wood – the bones move around with every step we take. At the same time, the skin, sock and shoe tend to stay stuck in stationary contact with one another. Essentially, the skin and bones move out of sync. When a bone moves, it pulls on the soft tissue it’s attached to. Therefore, the problem of blisters starts when you consider that every layer of soft tissue between bone and skin are structurally connected.
With the bone moving and the skin not moving, all the soft tissue in between stretches and distorts. This is called a shear distortion. It comes from one tissue layer sliding over another. Understandably, there is a finite amount that can occur before there is a tear in these connections, and this point will be different for everyone. Once the tear occurs, it slowly fills with fluid to resemble what we know and love as a blister. Blister prevention is all about either increasing the skin’s resilience to shear distortion, reducing the magnitude of shear distortions or reducing the number of shear distortions, or combinations of these.
Conclusion – The new blister paradigm
Blisters are a tear under the skin surface caused by the skin and bone moving out of sync. As the bones move within the foot with each step, the skin does not immediately follow. And so the soft tissues in between are made to stretch and distort. This is called a shear distortion. If there is too much shear, a tear develops under the skin surface which later fills with fluid to become what we recognise as a blister. The point at which the tear occurs under the skin surface is determined by, a) the number of shear distortions, b) the intrinsic resilience of the skin to shear distortion and, c) the magnitude of shear distortions.
Please, when describing blisters (what they are, what causes them) avoid any reference to heat, moisture, friction or rubbing. If you can do this, you’ll be helping to progress the way we understand how to effectively prevent and treat them.
References
- Comaish JS. Epidermal fatigue as a cause of friction blisters. Lancet. Published online 1973:81-83.
- Akers WA, Sulzberger MB. The Friction Blister. Mil Med. 1972;137(1):1-7.
- Naylor PFD. Experimental friction blisters. Br J Dermatol. 1955;(67):327–42.
- Knapik JJ, Reynolds KL, Duplantis KL, Jones BH. Friction Blisters: Pathophysiology, Prevention and Treatment. Sport Med. Published online 1995. doi:10.2165/00007256-199520030-00002
- Griffin CPT, Cortese TA, Layton LL, Sulzberger MB. Inverse time and temperature relationship in experimental friction blisters. J Invest Dermatol. 1969;52(Morning Session):384-401.
- Cortese TA, Griffin TB, Mc M, Layton LL, Hutsell TC. Experimental Friction Blisters In Macaque Monkeys. J Invest Dermatol. 1969;53(2):172-177.
- Patterson HS WT and LW. Foot blister risk factors in an ROTC summer camp population. Mil Med. 1994;159(2):130-135.
- Hashmi F, Richards BS, Forghany S, Hatton AL, Nester CJ. The formation of friction blisters on the foot: The development of a laboratory-based blister creation model. Ski Res Technol. 2013;19(1). doi:10.1111/j.1600-0846.2012.00669.x
- Knapik JJD. Friction Blisters: Pathophysiology, Risk Factors, And Prevention.
- Knapik J, Reynolds K, Staab J, Vogel JA, Jones B. Injuries associated with strenuous road marching. Mil Med. 1992;157:64–67.
- Covill D, Guan Z, Bailey M, Pope D. Effects Of Varying The Environmental Conditions On In-Shoe Temperature.
- Hall M, Shurr D, Zimmerman B, Saltzman C. Plantar Foot Surface Temperatures With Use Of Insoles. Iowa Orthop J. 2004;24:72-75.
- Deng F, Gong T, Jin H, Du S. Research on Factors Influencing Temperature and Relative Humidity Inside of Shoes.
- Naylor PFD. The skin surface and friction. Br J Dermatol. 1955;67:239-248.
- Nacht S, Close J-A, Yeung D, Gans EH. Skin friction coefficient: changes induced by skin hydration and emollient application and correlation with perceived skin feel. J Soc Cosmet Chem. 1981;32:55-65.
- El-Shimi AF. In vivo skin friction measurements. J Soc Cosmet Chem. 1977;(28):37-51.
- Kirkham S, Lam S, Nester C, Hashmi F. The effect of hydration on the risk of friction blister formation on the heel of the foot. Ski Res Technol. 2014;20(2):246-253. doi:10.1111/srt.12136
- Friction definition. Oxford Advanced Learner’s Dictionary. Accessed December 5, 2020. https://www.oxfordlearnersdictionaries.com/us/definition/english/friction?q=friction
- Sanders JE, Daly CH, Burgess EM. Interface shear stresses. J Rehabil Res Dev. 1992;29(4):1-8.
- Richie D. How To Manage Friction Blisters. Pod Today. 2010;23(6):42-49.
- Carlson JM. Functional Limitations From Pain Caused by Repetitive Loading on the Skin: A Review and Discussion for Practitioners, With New Data for Limiting Friction Loads. J Prosthetics Orthot. 2006;18(4):93-103.
- Yavuz M, Davis BL. Plantar shear stress distribution in athletic individuals with frictional foot blisters. J Am Podiatr Med Assoc. Published online 2010. doi:10.7547/1000116
- Sulzberger MB, Cortese TA, Fishman L, Wiley HS. Studies on blisters produced by friction I – Results of linear rubbing and twisting technics. J Invest Dermatol. 1966;47(5):456-465.
- Spence WR, Shields MN. Prevention of blisters, callosities and ulcers by absorption of shear forces. J Am Podiatr Med Assoc. 1968;58(10):428-434.
- Hoffman MD. Etiological Foundation for Practical Strategies to Prevent Exercise-Related Foot Blisters. Curr Sports Med Rep. 2016;15(5):330-335. doi:10.1249/JSR.0000000000000297





5 Responses
I am fascinated with this article. i developed a blister “out of the blue ” on my foot 2 weeks ago and two doctors and 1 podiatrist have no idea what it is. we have been peacking it to help with pain and now it is turning dark gray. A scan revealed nothing internally and there is no infection. The pain feels like a bruise.
All my life I’ve suffered with blisters on my feet. In the warmer weather I’ll get blisters on the bottom of my feet, on the soles and especially on the balls of my feet. The only solution for me is to avoid closed shoes in the summer months and limit my walking. Wearing running shoes will have me develop blisters in the matter of 20 minutes.
I’ve even developed blisters under tough skin and the blisters will end up growing inwards. I’ve even developed blisters inside of blisters in the span of 2 – 3 days.
Regardless it’s been really difficult being a prisoner to this condition.
What preventions have you tried? Read this if you don’t know where to start: https://www.blister-prevention.com/blogs/prevention/blister-on-bottom-of-foot
Hi Rebecca, the above comment is my patient. She is a young healthy person . Her blister is large and appeared overnight with no obvious cause. She first noticed some pain or sting in the area.
It is on her heel , no callus present. It’s not inflamed or swollen.
The fluid is quite deep. The doctor tried to aspirate it with not much success.
I have applied deflective padding to alleviate the pain.
Could a blister be caused by a bite from something ?
It doesn’t sound like a friction blister, which is the subject I am most knowledgeable about, Carin. Given that there is a single lesion, it sounds most like a bite. But there are many other causes/types of blisters. Read this for information. With your patient’s consent, you could also consider posting an image and history on the PDIG FB group for the group’s collective thoughts. Or, of course, referral to dermatology.