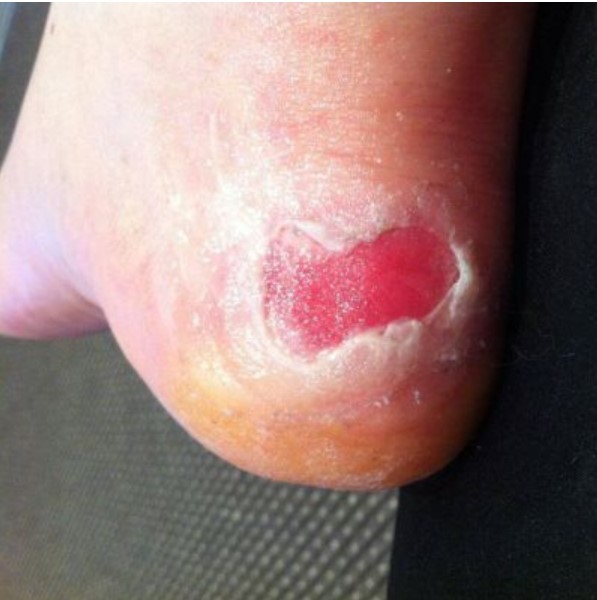
Foot ulcers, calluses and blisters… they’re all caused by the same thing. Repetitive shear deformation! The combination of:
- High friction force (pressure and coefficient of friction)
- Bone movement
Paralleles between foot ulcers, calluses and blisters
What I’d like to do is draw some parallels between what causes ulcers, calluses and blisters. Is it:
- Heat, moisture and friction that causes blisters?
- Pressure that causes callouses?
- Neuropathy and ischemia that causes ulcers?
No. It’s shear stresses. That’s the mechanics of it all. So what is this shear all about – because to me, shear used to be an abstract concept.
Not a block of wood
To understand, you just need to remind yourself that the foot doesn’t function like a block of wood. From heel strike to toe off, things move around in there. Bones move. All the squishy soft tissue layers move too. Just do this. There’s a fair bit of give in them – they stretch and distort, don’t they.
Forces in opposite directions
Shear is what happens when you have the bones of the foot moving one way. And the force of friction working the opposite way. And everything in between stretches. Shear is the parallel gliding of soft tissue layers over one another, to allow … this.
Barefoot heel strike
For simplicity’s sake, let’s imagine a barefoot heel strike.
- Your heel hits the ground.
- Friction keeps the skin stuck to the floor surface.
- Meanwhile, momentum makes the bones move forward, relative to the surface of the skin.
See that? Skin stays stuck, bones move forward, soft tissues in between stretch. Layer upon layer, they stretch and distort right? And when it happens too much or too far, it can cause blisters, callouses and ulcers, depending on other contributing factors.
Doug Richie DPM on shear
Doug Richie described shear nicely in his 2010 blister paper as “the skin and bones moving out of sync”. He’s describing how the skin surface remains stationary while the bones move back and forth. The result is all the soft tissues in between shear. Foot ulcers, calluses and blisters are all the result of this repetitive skin shear.
Not a loose bag of tissues
So while we know the foot isn’t a block of wood, it’s also not a loose bag of tissues where you can open the bag and simply pluck each item out individually. Everything between skin surface and bone is connected. So the amount of stretching that can occur before some of these connections break is finite. At some point, there will be a mechanical fatigue. Something will break if you exceed that threshold.
Blisters
When it comes to blisters, that mechanical fatigue occurs in the epidermis, below the skin surface a little bit – in the stratum spinosum. A tear occurs and within 2 hours it fills with fluid and resembles the blister we’re all familiar with.
When it comes to ulcers, the same thing happens. I’m no diabetes expert, but thinking about how diabetes increases the stiffness of connective tissue, there’s going to be less available stretch in the soft tissues layers before the injury threshold is reached. And especially so with scar tissue at previously healed ulcer sites.
Calluses
And when it comes to callouses, I’m not sure you’d call a callous an injury, but it is a hyperkeratotic lesion caused by excessive shear stress. Belinda Longhurst summarised it nicely for us on PodChatLive not long ago when she mentioned Farina Hashmi and Chris Nesters paper on callouses and explained that these excess shear forces result in incomplete corneocytes (skin cells) which because they’re incomplete, they’ve still got their nucleus in them so they’re a bit sticky and they clump together.
Demo – Contributing factors
Pressure
Firstly, we’re pressing with a certain pressure. Now let’s vary the pressure. If I press really hard, the magnitude of shear is high. But if I press really lightly, there’s very little shear before my fingertip slides or rubs across the skin surface.
Coefficient of friction
Secondly, there’s a certain slipperiness of stickiness between our fingertip and the back of our hand. If I reduce the COF levels with a lubricant, say like with this Aquaphor (which is similar to Vaseline), pressing with the same pressure as before leads to a much lower magnitude of shear. Even if I press really hard, shear distortions are way less than without the lubricant. If however I’d been in shoes and socks and exercising for a while, my skin would a bit clammy and sticky, which means a higher friction level. Using the same pressure would result in larger shear distortions in these soft tissues.
Bone movement
And thirdly, bone movement. The bones at the back of our hand are moving relative to the skin surface. Well in this case, we’re doing the opposite. To mimic the foot a little better, we’d keep our fingertip stationary and wobble our hand back and forth.
Summary
Foot ulcers, calluses and blisters have shear distortions as a common theme. If you can minimise the coefficient of friction, pressure and bone movement, you’ll be going a long way to reducing blister, callus and ulcer formation.